Department of Infectious Diseases and Microbiology (IDM) faculty members have been awarded more than $150 million in funding from the National Institutes of Health (NIH) and other agencies over the past 10 years. Since 2003, Pitt Public Health has consistently ranked third nationally in NIH funding among comparable institutions. Our research involves students, postdoctoral fellows, and highly trained research staff.
The following are examples of standout funded IDM faculty research.
Complications of Antiretroviral Therapy
Assistant Professor Jeremy Martinson is leading research on genetic factors affecting cardiovascular complications of HIV therapy. The introduction of Highly Active Antiretroviral Therapy (HAART) has transformed the lives of many HIV-positive individuals. For some, however, HAART carries a risk of cardiovascular side effects, although the etiology of this is unknown. HIV infection is known to contribute to cardiovascular disease risk in some patients. Martinson and his team are investigating the extent to which host genetics, HIV infection, and treatment with HAART interact to give rise to cardiovascular disease in patients enrolled in the Multicenter AIDS Cohort Study. They are currently using a variety of high-throughput genomic and transcriptomic approaches to study this phenomenon.
HIV-1 Associated Neuropathogenesis and 3D Brain Organoid Models to Study Neurodegenerative Diseases and Therapeutic Strategies to Mitigate Chronic Inflammation
HIV-associated neurocognitive impairment (HAND) is commonly observed in AIDS patients worldwide. During early infection, HIV-1 enters the Central Nervous System (CNS) and resides in macrophages/microglia and causes neuronal degeneration and inflammation in the brain. HAART therapy has improved the quality of life and longevity of HIV-1 infected patients; however, with aging, the prevalence of HAND is high in this population. Velpandi Ayyavoo’s laboratory focuses on understanding how HIV-1 induces neuronal dysfunction and destruction and how to detect them during the early stages as neurodegeneration occurs over a long period of time resulting in clinical manifestations. However, studying brain pathologies are complicated due to the lack of physiologically relevant models with encompasses the cell lineages including neurons, astrocytes and glia. Thus, her laboratory has developed a 3D-brain organoid model that will enable studies to delineate neurodegenerative diseases (Reis et al. 2020, Scientific Reports). Using this model her group is focusing on addressing how HIV infection induces chronic inflammation in the CNS and the consequences of inflammation on neurons and other bystander cells in the brain. Additionally, research is focused on developing immunotherapeutic treatment strategies that will reduce infection induced inflammation by overexpressing microRNAs that could potentially block inflammatory factors. The therapeutic potential of these miR-microglia will be assessed in the 3D-organoid model and in humanized mouse model.
AIDS Education and Prevention
“Disparities in health care, the stigma of HIV/AIDS, and the need for more timely testing and treatment are still barriers to delivering and improving HIV care,” said Linda Frank, associate professor. Frank is a principal investigator at the Pennsylvania/MidAtlantic AIDS Education and Training Center, headquartered at Pitt Public Health since 1988. The center is a national leader in supporting the training and education of health professionals who care for the thousands of people infected annually with HIV in the United States. A recent grant will allow scientists like Frank to continue to provide critical training to health professionals to reduce barriers to HIV care, increase HIV testing, integrate HIV prevention into primary care, and improve linkages to HIV treatment and expert clinical management of HIV and other comorbid conditions, such as hepatitis, sexually transmitted infections, tuberculosis, and substance use.
Tuberculosis
Nearly one third of the world’s population is infected with Mycobacterium tuberculosis, the bacterium that causes tuberculosis (TB). Although the vast majority of M. tuberculosis-infected people never experience the clinical symptoms of TB, there are almost 11 million new cases of TB and two million TB-related deaths annually. HIV is strongly associated with active TB, even in individuals with well-preserved CD4+ T cell levels, and TB is the leading cause of death in HIV-infected individuals. The causes of active TB are poorly understood, but are likely to include changes in anti-mycobacterial immune responses in granulomas, the site of M. tuberculosis infection. Assistant Professor Josh Mattila and his lab are focused on understanding the immune environment in lungs and TB granulomas. His particular interest is examining interactions between myeloid cells, including macrophages and neutrophils, and T cells in this environment with the objective of identifying factors that differentiate pathologic and protective responses. T cells (red) and macrophages (green) are present in distinct regions in granulomas where they cooperate to control Mycobacterium tuberculosis infection.
Emerging Infections
I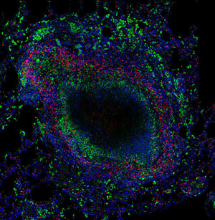 nfluenza virus is a respiratory pathogen that targets the lung, and innate immune responses serve a key role in providing early antiviral immunity and limiting disease in acute infection. However, the relationship between dendritic cells and immunity in the lung is not well defined. Professor Simon M. Barratt-Boyes and his team have used the murine model to examine the impact of plasmacytoid dendritic cells in the early immune response to influenza virus infection. They are also studying the dynamics of the dendritic cell response to avian influenza virus infection in the lung of nonhuman primates, which they believe serves as a more robust model of influenza in humans than do mice.
nfluenza virus is a respiratory pathogen that targets the lung, and innate immune responses serve a key role in providing early antiviral immunity and limiting disease in acute infection. However, the relationship between dendritic cells and immunity in the lung is not well defined. Professor Simon M. Barratt-Boyes and his team have used the murine model to examine the impact of plasmacytoid dendritic cells in the early immune response to influenza virus infection. They are also studying the dynamics of the dendritic cell response to avian influenza virus infection in the lung of nonhuman primates, which they believe serves as a more robust model of influenza in humans than do mice.
HIV Prevention and Planning
The HIV Prevention and Care Project (HPCP) is one of the longest running technical support and HIV planning programs for any statewide jurisdiction in the United States. Founded in 1992, the program has generated more than $40 million dollars in state and federal pass through funding to engage and empower people living with HIV, organizational stakeholders, and communities impacted by or at-risk from HIV. With a staff of more than 15 scientists, trainers, stakeholder engagement specialists, and technical experts, the HIV Prevention and Care Project collaborates with the Pennsylvania Department of Health’s Division of HIV Disease and related state agencies to provide organizing support, meeting facilitation, scientific expertise, intervention delivery, community advisory board development and maintenance, pilot programs and community-based research for some of Pennsylvania’s most vulnerable communities, and capacity building and technical assistance for the Commonwealth of Pennsylvania.
HPCP's models for achieving integrated HIV prevention and care planning for structural, meaningful involvement of most-at-risk communities in these processes have been cited as best practices by federal entities including the Health Services and Resources Administration, Centers for Disease Control and Prevention, and NASTAD. Sarah Krier serves as PI and David Givens and Teagen O'Malley are co-PIs.
Some previous and ongoing HPCP intervention projects include:
Project Silk
(CDC demonstration project)
A recreation-based community health center for young men (13 to 29 years) who have sex with men (MSM) and transgender women of color. Diffusion of Project Silk throughout PA with locations in Pittsburgh, Lehigh Valley, and Harrisburg.
Acceptance Journeys Pittsburgh
A social marketing intervention geared towards addressing and reducing stigma associated with lesbian, gay, bisexual, transgender, and queer (LGBTQ) individuals. The project invites individuals outside of the LGBTQ community to share their stories of love and acceptance of someone who is LGBTQ.
STD-to-PREP
(CDC demonstration project)
A data-to-prevention approach for increasing PrEP access and individualized HIV prevention navigation for under-served populations in Allegheny County.
PA Intersectional Stigma
A state-wide phased project using stakeholder-engaged approaches to document the impact of intersectional stigma in health care settings among people living with HIV, determine health care agencies readiness for stigma reduction efforts, co-design interventions for HIV care settings, and pilot intervention concepts throughout PA.
HIV Self-Testing
A state-wide initiative to expand HIV testing to communities with limited access to testing services with free at-home self-test kits.